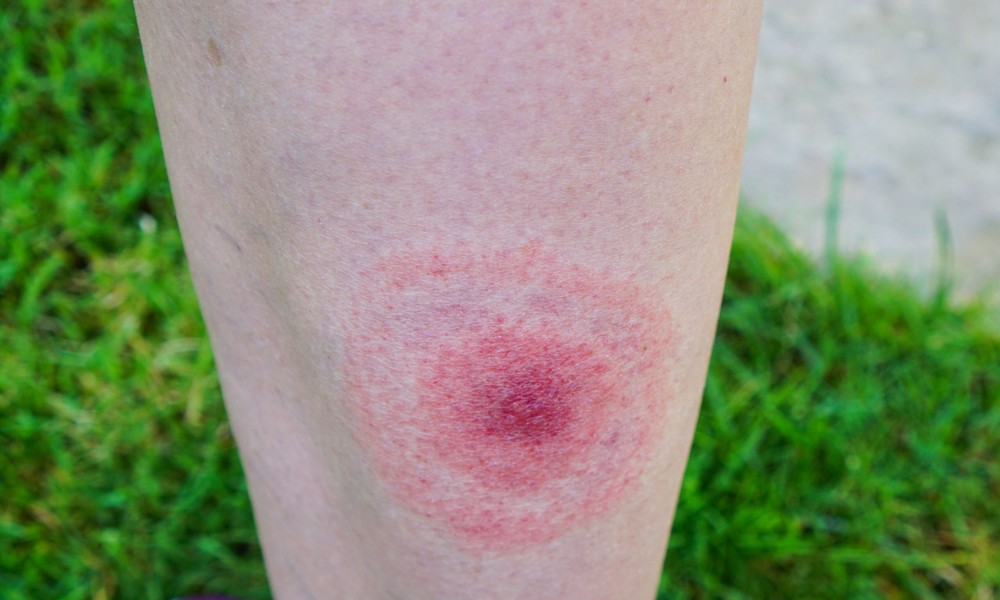
Skin rashes are often dismissed as allergic reactions, infections, or temporary irritations. However, persistent or atypical rashes may indicate underlying systemic issues that require more than a temporary treatment.
Dermatologists and rheumatologists from many hospitals often collaborate to uncover internal causes of skin symptoms.
In Singapore, patients with unexplained or recurring rashes may be referred across specialities to identify if an underlying autoimmune or inflammatory condition is at play.
When Skin Symptoms Point to Systemic Illness
Rashes caused by systemic conditions usually don’t resolve with standard dermatological care. A dermatologist in Singapore may begin to suspect an internal cause when a patient’s rash is widespread, recurrent, or linked with symptoms like joint pain, fever, fatigue, or muscle weakness. For instance, conditions such as lupus, dermatomyositis, and vasculitis often present with distinct skin patterns. A malar rash across the cheeks, for example, is strongly associated with systemic lupus erythematosus (SLE). Once a skin presentation suggests such a condition, the dermatologist refers the patient to a rheumatologist for further investigation.
What a Rheumatologist Investigates Beyond the Skin
A rheumatologist assesses whether the rash is connected to an autoimmune disease affecting joints, muscles, and internal organs. Rheumatologists in the city-state routinely encounter patients referred from dermatology who show signs of connective tissue disorders. Blood tests are often ordered to detect markers of inflammation, autoantibodies, and organ function. For example, elevated antinuclear antibodies (ANA) may indicate lupus or another connective tissue disease. Rheumatologists also examine other non-skin symptoms, joint stiffness, morning pain, dry eyes, and mouth ulcers, which help confirm a systemic diagnosis.
Key Conditions That Require Joint Dermatology-Rheumatology Assessment
There are several conditions where both specialities need to be involved. Psoriatic arthritis, for instance, requires management of both skin plaques and joint inflammation. A dermatologist may treat the visible symptoms, but without rheumatology intervention, joint damage could progress. Dermatomyositis is another key example; it presents with distinctive rashes on the eyelids and knuckles, often accompanied by muscle weakness. Prompt coordination between dermatology and rheumatology ensures early treatment to reduce long-term complications. Similarly, systemic sclerosis (scleroderma) starts with skin thickening but evolves into vascular and internal organ involvement, necessitating dual-specialist management.
Diagnostic Tools and Clinical Collaboration
The patient journey, in practice, often starts with a general practitioner or dermatologist, who conducts skin examinations and may perform a biopsy. Many dermatologists are trained to spot signs of systemic disease and have established referral pathways with rheumatology clinics. Some tertiary hospitals and private medical centres offer multidisciplinary clinics where dermatologists and rheumatologists co-manage complex cases. Imaging tests, skin histopathology, immunology panels, and joint assessments are used to build a comprehensive diagnosis. Treatment plans often include both immunosuppressants and targeted skin therapies.
When to Consider Seeing a Specialist for Your Rash
Patients who notice skin symptoms that don’t respond to typical creams, or who develop systemic signs alongside rashes, should consult a dermatologist promptly. Early referral to a rheumatologist is advised if there is suspicion of autoimmune or inflammatory disease. Waiting for symptoms to progress before seeing a specialist may result in organ damage or irreversible joint complications. Common red flags include rashes with joint swelling, skin ulcers, persistent facial redness, or symmetrical lesions that return periodically.
Conclusion
Not all rashes are skin-deep. Some are early signs of complex systemic disorders that necessitate both dermatological and rheumatological care. Collaboration between dermatologists and rheumatologists enables proper diagnoses and comprehensive treatment. It may be time to look beyond the surface if your skin condition is resistant to standard care.
Worried that your rash may signal something more serious? Visit the National University Hospital (NUH) and let us help you manage autoimmune conditions properly.